Manifestations of Candida mycoses
As a commensal organism, Candida is very commonly found on the human skin and mucous membranes. Changes to the external conditions lead to an increase in growth of Candida and to the extent of clinically relevant symptoms of a yeast infection.
Clinical manifestations of mycoses are to be found on all areas of the skin and mucous membranes, as well as in the gastrointestinal tract.
Oral thrush and diaper rash
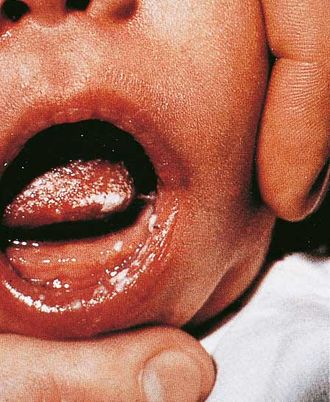
Oral thrush: Already during birth, neonates can come into contact with yeasts from the mother’s vagina. Later on, bottle teats, breast pumps, toys and other objects surrounding the child are often the source for mycoses. Yeasts can colonise on the skin and in the mouth of children and lead to inflammation and erosion of the epithelium. They can sometimes multiply and spread in the mouth and throat so profusely that visible white patches or plaques can be seen. This oral thrush (also known as “oropharyngeal candidosis”) can also arise in older patients and those with weakened immune systems.
Diaper dermatitis: Waterlogging and warmth favour yeast infections. Thus, the typical picture of diaper dermatitis in infants and small children arises with a diffuse, varnish-like glossy redness in the genital and anal region. In addition, large macerations occur with partly flaming red and wet erosions, which are very painful for the child.
Candidosis intertriginosa and Candidosis interdigitalis
Mycosis of the large skin folds (Candidosis intertriginosa): Candidosis intertriginosa is one of the most frequent fungal infections of the skin. Older people in particular are often affected. The warm, moist conditions in the large skin folds, e.g. in the groin, beneath the breasts or the belly or in the armpits, favour Candidosis intertriginosa. Infestation is characterised by exuding, reddened areas with surrounding scaly zones and possibly severe itching.
It is advisable to assess the situation as the symptoms can also arise from allergic reactions or following bacterial infections.
Interdigital fungal infections (Candidosis interdigitalis): Candida infections of the interdigital spaces of the hands and feet are mainly caused by Candida albicans. Mycosis on the hands is favoured by permanent wetness and sweating. As such, it is particularly widespread in gastronomy with cooks, as well as in the sugar and fruit processing industries.
The third interdigital cleft of the hands and the space between the fourth and fifth toe is most frequently involved. Fungal infections of the feet are as well favoured by moisture caused by a strong tendency to sweat, or frequent working in a humid condition and/or in water.
Symptoms are softening, itching and cracking of the skin. If the sole of the foot is also affected, blistering, redness and scaling of the skin are additional characteristics.
Fungal infections of the gastrointestinal tract
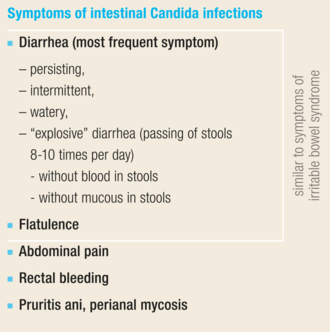
Fungal infections of the gastrointestinal tract: Candida ssp. can cause pathological effects in the entire gastrointestinal tract, especially in the lower region. As such, the symptoms of yeast infections are usually non-specific and can strongly resemble those of irritable bowel syndrome.
Pathogenesis of colitis
For colitis affecting the lower gastrointestinal tract in particular, a number of pathogenetic mechanisms are known.
Pathological effects in the lower gastrointestinal tract
- Enterocolitis following direct invasion of the mucosae of the small or the large intestines
- Diarrhea without substantiated invasion of the mucous membranes (mechanism not known)
- Ischaemic enteritis due to Candida sepsis and haematogenic spread (incl. the formation of embolisms)
Identification of intestinal yeast infections in diarrhea
In the presence of symptoms and the exclusion of the well-known pathogens causing diarrhea, the German Society for Hygiene and Microbiology (DGHM) defines an intestinal fungal infection as the detection of 105 or more yeast cells/g of stool. The additional determination of virulence factors (e.g. SAP) can provide further information about whether in this case, in the present of clinical symptoms, a fungal requires treatment.
Systemic Candida infections
Systemic Candida infections: A higher risk for invasive candidosis is to be found in patients in intensive care units, those with severely debilitated immune systems or endocrinopathies. The entry points for an invasive infection are existing Candida colonisations, e.g. on the skin, the oropharynx or the gastrointestinal tract.
In the case of limited immune competence, a weakening of the intestinal mucosal barrier (leaky gut) can help simplify the transfer of Candida antigens and their metabolic products into the blood circulation.
Haematogenic dispersal may lead to the development of sepsis and micro-abscesses with subsequent organ damage.
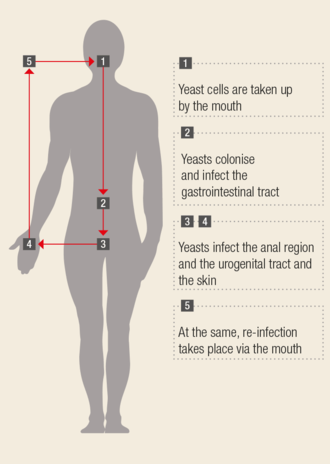
Cause of recurrent extra-intestinal yeast infections: the intestine as a reservoir for pathogens
The gastrointestinal tract acts as a reservoir for recurrent yeast infections. They are able to spread via the mouth as the gateway to infection throughout the entire gastrointestinal tract. The spread is through smear infections in the genital area and over the body’s entire surface. As a consequence, relapsing or chronic vaginal mycoses infections and genitourinary tract mycoses are able to occur, or in the case of children recurrent diaper dermatitis can arise. The vicious circle of infection and re-infection closes when the pathogens return to the mouth again. Only by a consequential clean-up of the entire gastrointestinal tract is it possible to effectively interrupt this cycle.